
Which Medical Coding & Billing Certification Exam Should You Take – the CBCS or CPC?
Certification is important for many healthcare fields, and medical billing and coding has several certifications to choose from. Learn more about CBCS, CPC, and CCA certifications and how they impact your career.
Jul 07, 2025
9 min read
We follow strict quality and ethics policies to make sure our content is honest, accurate, and helpful. Learn more about our editorial guidelines.
Medical billing and coding is a rapidly growing career field, with 191,500 jobs expected to open by 2033. Professionals in this industry can work for a variety of employers including hospitals, private practices, research firms, insurance companies, and more. Earning a medical billing and coding certification is required for most jobs in the field, but there are several exam options to consider. Learn the pros and cons of each and how to make the best decision for your career.
Why take a certification exam?
Certification may be preferred by many employers, and can help set you apart from others. Jaime Nguyen, MD, MPH, MS, Director of Healthcare Programs at Penn Foster Group, explains, “Medical coders continue to be in high demand and there’s a lot of opportunities for career growth. You can work in insurance billing and then in more specialized coding, such as obstetrics and orthopedics, and then advance to medical auditing and inpatient coding. Being certified is key to employment and advancement.”
“It is a good field to be in right now,” mentions Diana Murphy, a medical billing and coding instructor. “An individual working on getting their certification in coding and billing shows they are the professional a medical company would benefit from having on their team. The medical field needs individuals with knowledge on billing and coding and understanding the insurance world, ensuring proper reimbursement on claims.”
Earning a medical billing and coding certification is not necessarily required for most jobs in the field, but many employers prefer to hire certified medical billing and coding professionals. According to the National Healthcareer Association (NHA), 83% of employers state that they would hire a candidate with nationally recognized certifications over someone without.* Being certified can also have a positive impact on how much you can earn as a medical biller and coder, what jobs you qualify for, and can help you advance in your role. However, there are several different types of billing and coding certifications you can pursue, so deciding which to take can be confusing. Which one best fits you? Learn the pros and cons of each, which one is right for you, and how to make the best decision for your career.
Which coding certification is best?
There isn’t one specific certification that is necessarily considered the “best” overall. Each type of billing and coding certification offers different pros and cons, and different requirements. It’s more about choosing which certification best fits your goals and understanding which certifications you’re actually qualified to take. While there are many coding-specific certifications – even certifications for coding specialties – the most common exams are the following.
Read more: Your Medical Billing & Coding Salary Guide
1. Certified Billing and Coding Specialist (CBCS) Exam
The Certified Billing and Coding Specialist (CBCS) certification offered by the National Healthcareer Association (NHA) is designed to make sure medical billing and coding professionals know how to properly code for illnesses, procedures, and other common medical needs in accordance with insurance standards. The CBCS covers the broad, foundational skills that are vital to medical billers and coders who want to work in physician’s offices, hospitals, dental offices, nursing homes, insurance companies, and other medical facilities. The exam takes about 3 hours to complete, is 100 scored questions, and is timed. In order to take the exam, you’ll need to register on the NHA website. You’ll then have the option to take the test at a testing center near you or remotely. If you’re a Penn Foster Medical Billing and Coding Program graduate, the cost of your exam is covered by your tuition and prep materials are included so you can properly prepare to pass the test and become certified.
CBCS requirements: In order to sit for the CBCS, you need to be at least 18 years old, have a high school diploma or equivalent, and either have completed a medical billing and coding training program within the last 5 years or have at least 1 year of supervised work experience in the field.
Who is the CBCS right for? The CBCS exam is a great certification for someone new to the medical billing and coding field who wants to validate a broad range of essential, foundational coding skills.
Read more: Medical Billing & Coding Diploma Helps Grad Enter Growing Field
2. Certified Professional Coder (CPC) Exam
The Certified Professional Coder (CPC) certification offered by the American Academy of Professional Coders (AAPC) is the most popular medical billing and coding certification students pursue. The CPC concentrates on outpatient coding and covers how to assign diagnoses, procedures, and medical codes for an array of clinical services and cases. The exam is 100 multiple choice questions and test takers are allowed up to 4 hours to complete the exam. You’ll have the option to register to take the exam at a testing center near you or online. If you choose to take the exam online, you’ll need a reliable internet connection and external webcam. The AAPC offers a free exam retake, and many students participate in their local AAPC chapters.
CPC requirements: To sit for the CPC exam, you must be at least 18 years old and have a high school diploma. Additionally, you’ll need to have an active membership with AAPC, and they recommend those who take the exam have relevant work experience or education before taking the test.
Who is the CPC right for? The CPC exam is a great option for those who want to be a member of the AAPC, which offers networking opportunities and webinars to further your education.
Read more: Medical Billing and Coding Instructor Diana Strives for Quality of Care
3. Certified Coding Associate (CCA) Exam
The Certified Coding Associate (CCA) certification offered by the American Health Information Management Association (AHIMA) covers all-around coding across various settings including hospitals and physicians. This medical coding and billing certification validates your skills in coding procedures for recordkeeping, compliance, and confidentiality. The CCA is a timed exam and has between 90 and 115 total questions.
CCA requirements: There’s no minimum age requirement to be eligible to take the CCA certification exam. To qualify to sit for the exam, you just need to have a high school diploma or equivalent. AHIMA does recommend that you also have either 6 months of experience in the field or have completed an approved training course before taking the test, but it’s not required.
Who is the CCA right for? The CCA exam is a good fit for entry-level medical billers and coders who may not have completed an approved training course or are new to the field.
Read more: Jobs in Healthcare Management & Healthcare Administration: Your Career Guide
Is the CBCS a good certification?
Yes, the CBCS is a good certification to have as a medical billing and coding professional. Earning the CBCS credential proves that you have the necessary foundational skills in coding and healthcare to be an asset to any healthcare organization.
What comes after CPC certification?
After earning your CPC credential and beginning a job in the field, you may want to consider pursuing additional, advanced certifications. These additional certifications can help you advance in your career and even potentially help you earn more money. You may want to get your Certified Professional Biller (CPB) certification to add to your coding expertise. Or you may choose to specialize and become certified in a specific aspect of billing and coding such as inpatient or outpatient coding.
Read more: Does Education Make a Difference in Salary? (How Learning More May Help You Earn More)
Ready to Pursue Medical Billing and Coding?
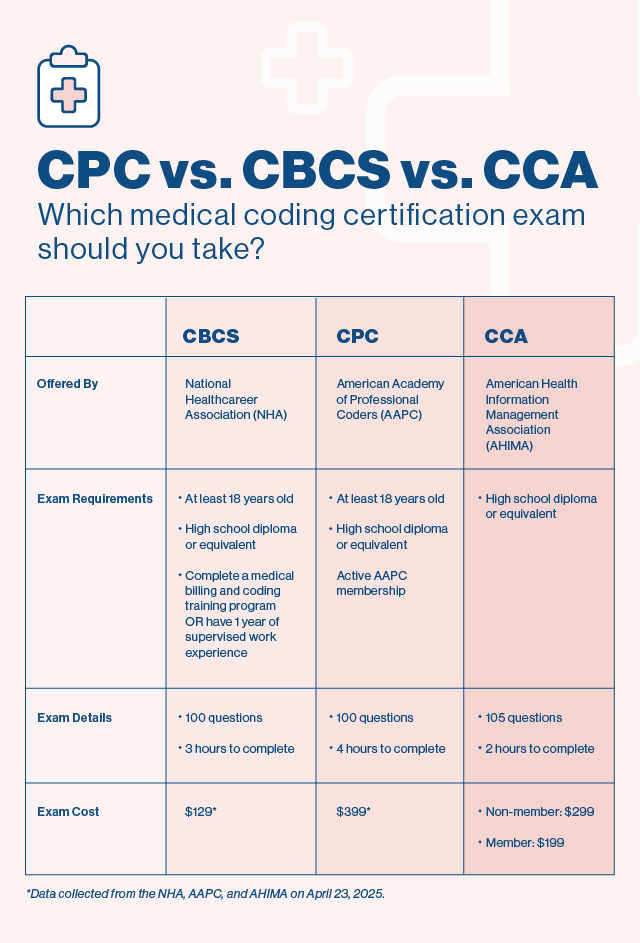
The Differences Between the CPC, CBCS & CCA
Becoming a certified medical billing and coding professional can be a great move for your career. While you can certainly take as many certification exams as you like – and it may seem like a great idea to add as many credentials to your resume as possible – the exams can be costly, usually hundreds of dollars.
Employers don't typically prefer one medical billing and coding certification over another, so it makes sense to choose one certification (at least at first) that feels like the best fit for you. Understanding the similarities and differences between the exams can help you narrow down your options.
The CPC and CCA are very versatile certifications that can be applied across multiple settings, while the CBCS may be more attractive to employers in the insurance industry. All three exams require a high school diploma or equivalent, with the CPC and CBCS requiring a minimum age of 18. All three are excellent starting points for students who eventually want to pursue a career in inpatient coding.
Jaime has this advice for those unsure which certification they should go for: “Which certification you choose may depend on what stage in your career you are and the type of healthcare setting you want to work in. The CPC certification is considered the ‘gold standard’ for medical coders. So, a good option for many students is to get the CBCS or CCA certification and then advance to get CPC certification. Another good thing is that you can complete the Medical Billing & Coding program and get your CBCS certification and then transfer some of your courses to the Medical Coding Professional program and get your CPC certification.”
Other differences include exam cost and experience requirements.
Read more: Medical Coding Professional vs. Medical Billing and Coding: What’s the Difference?
What coding specialty makes the most money?
The average salary for a certified medical billing and coding specialist is $50,250. Specializing in particular areas of billing and coding, however, can potentially allow you to earn even more! Specialties can include radiology, oncology, outpatient or inpatient coding, physician coding, and emergency coding.
In order to qualify for more advanced roles in the medical billing and coding field, such as becoming an emergency department coder, you may need to pursue further education and you will definitely need to earn additional credentials and certifications.
Read more: 5 Jobs You Need to Know About in 2025
Prepare for medical coding certification online
While not every certification exam requires you to have formal medical billing and coding training and education, most recommend it before attempting to take the test. Medical billing and coding is a complicated field that requires knowledge of standard coding procedures, medical codes found in the ICD-11 manual, and reimbursement methods. Having a formal education in the field can help you better prepare for certification exams and for the job! With an online program like Penn Foster’s Medical Billing and Coding Career Diploma, you can learn the foundational skills and knowledge that can help you take the next steps toward a rewarding healthcare career – from home, at your own pace.
Penn Foster Medical Billing and Coding graduate Rachel Delgado was ready to sit for her certification exam as a result of completing the online program and was even able to apply for roles in university hospital settings after she graduated! The program is designed to prepare you for the most recognized industry exams like the CBCS, CPC, and CCA!
To learn more about starting your medical billing and coding training today, request more information, enroll online, or reach out to our Admissions Specialists at 1-888-427-6500.
*National Health Career Association. “2024 Industry Outlook.” nhanow.com. January 22, 2024.



